|
www.HealthyHearing.com |
Middle ear infections
By Joy Victory, managing editor, Healthy Hearing  Reviewed by
Gillian Diercks, MD, MPH, pediatric otolaryngologist, Mass Eye & Ear Reviewed by
Gillian Diercks, MD, MPH, pediatric otolaryngologist, Mass Eye & Ear Last updated on: December 18th, 2024 Middle ear infections can cause temporary hearing loss in children. Learn the symptoms and find out when to seek medical help for your child. Key points:
Ear infections are common condition, especially among children. In fact, 5 out of 6 children will experience at least one ear infection by the time they are three. However, they can happen at any age. While there are several types of ear infections, middle ear infections are the most common. With a middle ear infection, the infection resides behind the ear drum, causing inflammation, pressure, and fluid build-up. This can affect hearing and cause intense pain. Symptoms of middle ear infectionsBabies and toddlersFor babies and toddlers who cannot talk, it can be hard to see the symptoms of an ear infection. If concerned, look for these tell-tale signs:
Kids, teens and adultsFor older children, adolescents and adults, these symptoms are also possible:
If you or your child has any of the symptoms above, call your pediatrician, family doctor or otolaryngologist, also known as an ear-nose-throat doctor (ENT). It is important to act quickly because a middle ear infection can easily be treated and the ear pain alleviated. Can ear infections cause hearing loss?Yes. Many different ear infections can affect hearing in one or both ears. This can be unsettling, but it's almost always temporary, mild, and doesn't result in any permanent hearing loss. Even so, a healthcare professional should evaluate any hearing loss, especially in kids. Addressing hearing loss is important because infants and toddlers who suffer from recurrent ear infections or chronic fluid in the ear following infection experience stretches of hearing loss. This can disrupt a critical period for developing speech and language skills, and impact their long-term communication abilities. Why do ear infections affect hearing?
During or after the initial infection, fluid can build up in the air-filled space behind the eardrum, which is known as otitis media with effusion. This build-up can reduce movement of the eardrum and middle ear bones, leading to trouble hearing. However, with proper treatment, the infection will clear and hearing should go back to normal. Can ear infections cause permanent hearing loss?While hearing loss from ear infections is almost always temporary, chronic untreated ear infections do carry a small risk of permanent hearing loss. This typically happens when the middle ear structures, like the eardrum or ossicles, are damaged after repeated infections and fluid buildup. Causes of middle ear infectionsMiddle ear infections usually happen during or after upper respiratory infections. They are often caused by viruses, like the common cold. The respiratory infection causes swelling and inflammation in the back of the nose and throat. This includes the opening of the eustachian tube. This tube links the throat to the middle ear. When it swells, it cannot balance the pressure in the middle ear. This is a type of eustachian tube dysfunction. When this pressure builds up, normal secretions can’t drain away as they usually would. The negative pressure and excess fluid can lead to an infection. 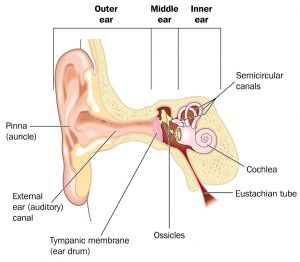
fluid can accumulate—causing pain, pressure and infection. Why are children so prone to ear infections?Younger children are far more prone to middle ear infections than others for two reasons. First, their immune systems are less developed, so it’s harder to fight off respiratory infections. Second, the eustachian tubes of young children are smaller and positioned more horizontally, making it harder for fluid to drain properly. Another risk factor for children is a chronic infection or enlargement of the adenoids. Adenoid tissue is located at the back of the nose next to the eustachian tubes, so viral or bacterial invaders can easily spread to the middle ear. Additionally, enlarged adenoids can block the eustachian tube openings, making it difficult for the tubes to function properly. Testing for an ear infectionAs part of a medical exam, a doctor will use a lighted otoscope to look inside the ears. In some cases, they may perform a tympanometry test to measure the health of the eardrum and middle ear. How are ear infections treated?Treating a middle ear infection usually involves two steps:
Doctors sometimes wait to prescribe antibiotics because an otherwise healthy child may be able to fight the infection on their own, helping to avoid any potential side effects and other risks of antibiotics. The American Academy of Pediatrics recommends focusing on pain management for the first 1 to 2 days before prescribing antibiotics. Over-the-counter ibuprofen and acetaminophen are recommended for pain relief, and occasionally ear drops that contain pain medicine.
If a doctor prescribes antibiotics to treat a middle ear infection, the first medication often prescribed is typically amoxicillin, as long as the child does not have a penicillin allergy. This oral antibiotic works to treat the infection. Over time, inflammation will get better, and the eustachian tubes can properly ventilate the middle ear. Until the backed-up fluids clear and the eustachian tubes function properly, your child may experience more infections and difficulty hearing. It is important to take the entire course of prescribed antibiotics—even if symptoms have subsided. Older children may report being able to hear better several days after they have resumed normal activities. This sign indicates that the fluid build-up has resolved. Treatment options for recurrent or chronic infectionsIf you or your child deal with recurrent middle ear infections and lingering middle ear fluid that affects hearing, an otolaryngologist may recommend a minor surgical procedure known as ear tube surgery to insert tubes into the eardrums. This is the most common outpatient procedure performed on children in the United States every year. During the procedure, an otolaryngologist will typically make a small cut in the eardrum. This cut is called a myringotomy. They will remove any fluid left in the middle ear. Then, they will place a small tube, known as a tympanostomy tube, into the eardrum. The tube, also called a pressure equalization tube, aerates the middle ear space through the ear canal. This allows trapped fluids to escape and helps prevent infections from coming back. This procedure is for children who suffer from ongoing infections even after using antibiotics. This means more than 3 infections in 6 months or 4 in 12 months with a recent infection. It's also recommended for children with middle ear fluid that lasts more than 3 months and causes hearing loss. Additionally, your surgeon may consider an adenoidectomy (removal of the adenoids) if there are symptoms of chronic stuffy nose or mouth breathing in addition to recurrent ear infections or persistent fluid in the middle ear space. Can you prevent ear infections?Because colds are very infectious, you can't fully prevent your child from getting sick. However, there are risk factors you can control:
Seek help for any hearing lossIf your child has sudden hearing loss but no signs of a middle ear or respiratory infection, seek immediate medical attention to ensure that nothing more serious is going on. There are many causes of hearing loss in children, and it's important to act quickly because children with hearing loss can have delayed language and speech development. Our directory can also help you find audiologists near you. This article has been medically reviewed by Gillian Diercks, MD, MPH, a fellowship-trained pediatric otolaryngologist at Mass Eye and Ear who sees pediatric patients at the Boston Main Campus and in our Newton and Wellesley practices. Dr. Diercks specializes in general pediatric ear, nose, and throat care, hearing loss, pediatric thyroid and endocrine disorders, treatment of sinus conditions and throat and voice care. Joy Victory, managing editor, Healthy Hearing
You are reading about: Related topics More information about hearing aids, hearing aid brands, assistive devices and tinnitus. Featured clinics near me
Earzlink Hearing Care - Reynoldsburg
HearingLife - Pickerington Find a clinicWe have more hearing clinic reviews than any other site! Related contentThe Healthy Hearing Report |
|
www.HealthyHearing.com |
Middle ear infections
By Joy Victory, managing editor, Healthy Hearing  Reviewed by
Gillian Diercks, MD, MPH, pediatric otolaryngologist, Mass Eye & Ear Reviewed by
Gillian Diercks, MD, MPH, pediatric otolaryngologist, Mass Eye & Ear Last updated on: December 18th, 2024 Middle ear infections can cause temporary hearing loss in children. Learn the symptoms and find out when to seek medical help for your child. |


 Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.
Joy Victory has extensive experience editing consumer health information. Her training in particular has focused on how to best communicate evidence-based medical guidelines and clinical trial results to the public. She strives to make health content accurate, accessible and engaging to the public.